CCCA (Central Centrifugal Cicatricial Alopecia)
What Is CCCA?
Central centrifugal cicatricial alopecia — CCCA — is the most common form of scarring hair loss in Black women. It begins at the crown (vertex) of the scalp and spreads outward in a centrifugal pattern, gradually destroying hair follicles and replacing them with scar tissue. The word “cicatricial” means scarring, and that distinction is critically important: unlike androgenetic alopecia or telogen effluvium, where the follicles are miniaturized or resting but still alive, in CCCA the follicles are permanently destroyed. Once a follicle has scarred, it cannot be revived.
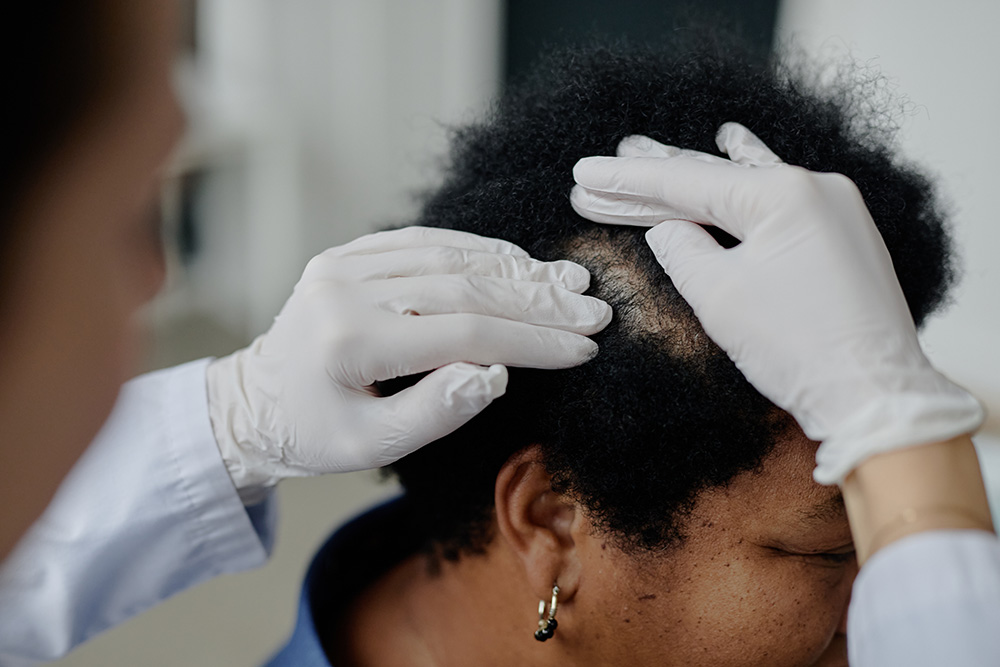
This is why early diagnosis and treatment matter so much.
The goal of therapy is to halt the inflammatory process before more follicles are lost — to preserve what is still viable. Treatment started early in the disease course can meaningfully change the outcome. Treatment delayed allows irreversible damage to accumulate silently.
Who Is Affected?
CCCA predominantly affects women of African descent. Estimates suggest it may affect up to 15% of Black women in the general population, though the true prevalence is likely higher because the condition is significantly underdiagnosed. Many women attribute early crown thinning to “stress” or “normal aging” and do not seek evaluation until the loss is advanced.
The condition typically presents in the third to fifth decade of life, though it can occur earlier. There is emerging evidence that CCCA may be associated with uterine fibroids, suggesting a shared inflammatory or genetic predisposition — though the exact link remains under investigation.
Causes: Genetics and Environment
The cause of CCCA is not fully understood, but the current evidence points to a combination of genetic susceptibility and environmental triggers.
On the genetic side, a landmark study published in the New England Journal of Medicine identified mutations in the PADI3 gene — which encodes an enzyme involved in hair shaft formation — as a significant risk factor for CCCA. This suggests a structural vulnerability in the hair follicle that predisposes it to inflammation and scarring.
On the environmental side, certain hair care practices may contribute to disease activity in genetically susceptible individuals. High-tension hairstyles, chemical relaxers, frequent heat styling, and the use of certain hair products have been associated with CCCA in observational studies. It is important to be clear about what this means and what it does not: hair care practices do not cause CCCA. They may, however, exacerbate inflammation in follicles that are already genetically vulnerable. Modifying these practices is part of the treatment plan, but blaming hairstyling alone oversimplifies the disease and unfairly burdens patients.
Symptoms
CCCA often begins insidiously. Many patients report gradual thinning at the crown that they initially attribute to aging or stress. Over time, the thinning spreads outward in a roughly circular pattern. The scalp in affected areas may appear shiny and smooth, with visible loss of the tiny openings (follicular ostia) where hairs normally emerge.
Some patients experience tenderness, itching, or burning at the crown — symptoms that indicate active inflammation. Others have no symptoms at all, which can delay diagnosis. Small papules (bumps) at the periphery of the affected area are another sign of active disease.
Diagnosis
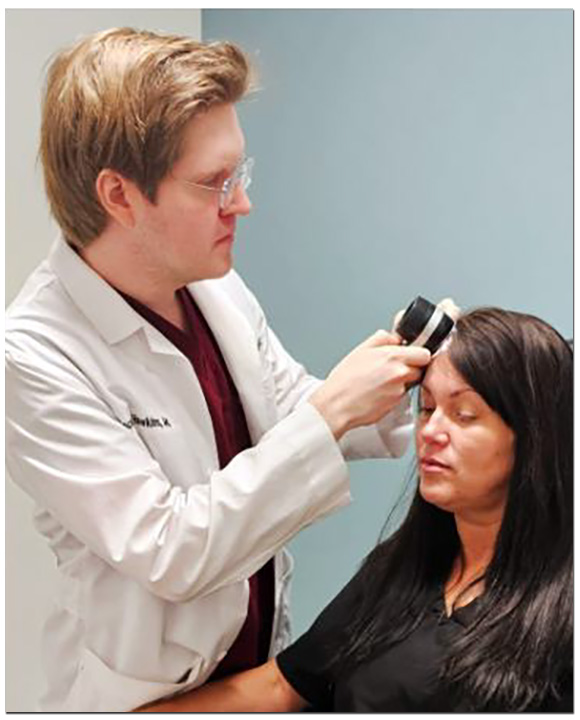
CCCA is diagnosed by a dermatologist through clinical examination, dermoscopy, and when necessary, scalp biopsy. Dermoscopic findings include loss of follicular ostia in the central zone, a gray-white peripilar halo (the “premature desquamation of the inner root sheath” finding characteristic of CCCA), and scattered broken hairs.
A scalp biopsy may be performed when the clinical picture overlaps with other forms of scarring alopecia (such as lichen planopilaris) or when the diagnosis is uncertain. The biopsy shows a pattern of lymphocytic inflammation centered around the lower portion of the follicle, premature desquamation of the inner root sheath, and progressive fibrosis replacing the follicular unit.
Accurate diagnosis is essential because the treatment approach for CCCA differs from other scarring alopecias, and misdiagnosis — or missed diagnosis — means lost time and lost follicles.
Treatment Approach
Anti-Inflammatory Therapy
The first priority is stopping the inflammatory process that is destroying follicles. Intralesional corticosteroid injections (triamcinolone acetonide) delivered directly into the affected scalp areas are a mainstay of treatment. These are typically administered every 4–8 weeks and provide targeted, potent anti-inflammatory effect with minimal systemic absorption.
At home, patients are often prescribed a rotation of topical clobetasol (a high-potency corticosteroid) and a topical JAK inhibitor, alternating between the two. This approach provides continuous anti-inflammatory control while minimizing the risk of skin atrophy associated with long-term use of any single topical steroid. For patients with significant active inflammation, oral doxycycline may be added for its anti-inflammatory properties (independent of its antibiotic activity).
Metformin — both topical and oral formulations — has emerged as an additional treatment option for CCCA. While traditionally used for diabetes, metformin has anti-inflammatory and antifibrotic properties that may help slow the scarring process. Its use in CCCA is relatively new but represents a promising avenue, particularly for patients who need additional disease control beyond standard anti-inflammatory therapy.
Systemic Therapy for Ongoing Control
For patients with aggressive or widespread disease, systemic immunosuppressive therapy may be necessary to achieve adequate control. Options include hydroxychloroquine, mycophenolate mofetil, and in refractory cases, other immunomodulators. These carry more significant side-effect profiles and require monitoring, but they can be essential for patients whose disease is not adequately controlled with topical and intralesional therapy alone.
Medical Therapy to Preserve Remaining Hair
While anti-inflammatory treatment stops the destruction, medical therapy supports the surviving follicles. Oral minoxidil helps stimulate growth in follicles that are weakened but not yet scarred. This can meaningfully improve density in areas at the periphery of the scarred zone where follicles are still viable.
Hair Care Modifications
Gentle hair care is an integral part of the treatment plan. This means reducing or eliminating chemical relaxers, minimizing heat styling, choosing lower-tension hairstyles, and being mindful of products applied to the scalp. These changes do not cure CCCA, but they reduce the external stressors on already-vulnerable follicles and create a more favorable environment for treatment to work.
This is not about telling patients what they cannot do with their hair. It is about collaborative problem-solving — finding styles that are protective, culturally appropriate, and compatible with scalp health. Dr. Hawkins is a speaker for the STRAND Network, a program that connects dermatologists and hairstylists to coordinate hair care practices for patients with medical hair conditions. Many patients find that working with a stylist who understands their diagnosis helps them maintain a sense of personal style while protecting their follicles.
Ongoing Monitoring
CCCA is a chronic condition that requires long-term follow-up. Even after the active inflammation has been controlled, periodic monitoring with dermoscopy helps detect early signs of flare before significant new damage occurs. Treatment is often tapered to a maintenance regimen rather than stopped entirely.
Distinguishing CCCA from Similar Conditions
Crown thinning in Black women can result from several overlapping conditions, and accurate diagnosis is essential because the treatment approach differs for each. Traction alopecia, caused by chronic mechanical tension from tight hairstyles, often coexists with CCCA and shares some of the same risk factors. However, traction alopecia primarily affects the hairline and temples (areas of greatest tension), while CCCA is centered at the vertex. Androgenetic alopecia can also cause vertex thinning in women, but it involves follicle miniaturization rather than scarring — the follicular ostia remain intact on dermoscopy.
Lichen planopilaris is another scarring alopecia that can occasionally overlap with CCCA, particularly in patients of African descent. Biopsy can help differentiate these conditions when clinical and dermoscopic findings are ambiguous. The treatment implications are significant: while both are scarring processes, the specific anti-inflammatory regimens differ.

Living with CCCA
CCCA is a chronic condition, and coming to terms with that reality is part of the treatment process. Many patients feel a sense of loss not just of hair, but of styling freedom and identity. These feelings are valid and worth acknowledging. At the same time, effective treatment can halt progression, medical therapy can thicken surviving hair, and surgical restoration can meaningfully improve density in appropriate candidates.
Connecting with other women managing CCCA — through support groups, online communities, or referral resources from your dermatologist — can help normalize the experience and provide practical advice on styling, camouflage, and coping. Camouflage tools including hair fibers (such as Toppik), strategic parting, and in stable cases, carefully applied hairpieces can provide cosmetic coverage during treatment.

Hair Transplantation in CCCA
Hair transplantation can be a meaningful option for patients with stable, quiescent CCCA who want to restore density to scarred areas. The critical prerequisites are at least 12 months of documented disease stability (no active inflammation, no new areas of loss) and a clear understanding that transplanted hair placed into a scarring environment carries some risk of future loss if the disease reactivates.
This is an area where having a dermatologist perform the transplant — rather than a surgeon from another specialty — provides meaningful safety. A dermatologist trained in both hair loss diagnosis and surgical restoration can accurately assess disease activity, make informed judgments about surgical timing, and provide ongoing medical management in conjunction with the surgical plan. Most non-dermatologist transplant surgeons do not routinely evaluate or treat CCCA and may not recognize signs of active disease.
Next Steps
If you are experiencing thinning at the crown — particularly if it has been gradually worsening, or if you have noticed tenderness, itching, or burning in that area — a comprehensive evaluation by a dermatologist experienced in scarring alopecia can determine whether CCCA is the cause and, if so, what stage you are in. Earlier treatment means more follicles preserved. At Hair Medicine Institute, Dr. Hawkins provides the full continuum of CCCA care: accurate diagnosis, medical and regenerative therapy, ongoing monitoring, and when appropriate, surgical restoration.
Without Treatment,
Your Hair Loss Will Continue.
Get a personalized treatment plan and get your hair back.
