There are treatment options for women experiencing Hair Loss.
You don’t have to accept losing your hair. We offer proven holistic hair-health solutions designed specifically for women.
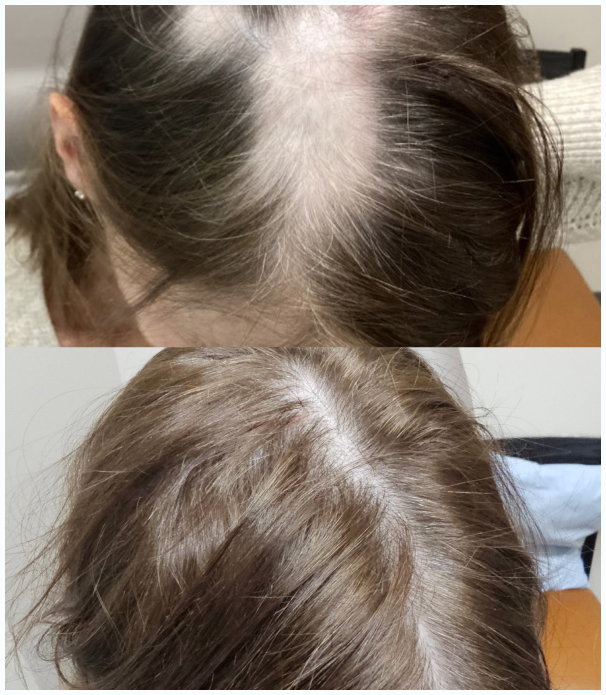
What Is Female Pattern Hair Loss?
Female pattern hair loss — clinically termed androgenetic alopecia — is far more common than most women realize. By some estimates, it affects up to 40% of women by age 50, and the prevalence increases significantly after menopause. Yet it remains underdiagnosed, undertreated, and frequently dismissed. Many women who seek help are told “it’s just stress” or “there’s nothing we can do” — neither of which is accurate.

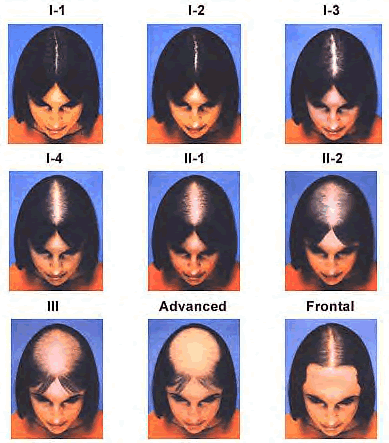
Female pattern hair loss presents differently from its male counterpart.
Rather than the frontal recession and vertex balding typical of male AGA, women most commonly experience diffuse thinning centered over the crown and mid-scalp. The frontal hairline is usually preserved.
The classic clinical sign is a progressively widening part. Over time, the scalp becomes visible through the hair, and overall hair volume and density decline. The Ludwig scale classifies the severity: Grade I (mild thinning), Grade II (moderate widening), and Grade III (significant thinning with visible scalp).
The Hormonal Landscape
The underlying mechanism shares similarities with male AGA — androgen-mediated miniaturization of genetically susceptible follicles — but the hormonal context in women is more nuanced.
Women produce androgens (testosterone, DHEA-S) from the ovaries and adrenal glands, though at much lower levels than men. Even at these lower levels, androgens can drive follicular miniaturization in genetically predisposed individuals. Conditions that increase androgen levels or androgen sensitivity — such as polycystic ovary syndrome (PCOS), adrenal hyperplasia, or androgen-secreting tumors — can accelerate or unmask hair loss.
Estrogen plays a protective role, prolonging the anagen (growth) phase and buffering the effects of androgens on the follicle. This is why many women notice their hair is thicker during pregnancy (when estrogen levels are high) and thinner after menopause (when estrogen declines and the relative influence of androgens increases). The postpartum period is a double hit: the estrogen drop triggers telogen effluvium (acute shedding), which can unmask previously subclinical androgenetic alopecia that was being masked by the hormonal environment of pregnancy.
This TE-AGA overlap is one of the most common and most missed diagnoses in women’s hair medicine. The telogen effluvium resolves, but the hair never returns to its pre-pregnancy density — because the underlying AGA was there all along.
Getting the Right Diagnosis
A proper evaluation for female hair loss is more than a glance at the scalp and a reassurance. It requires a systematic approach.
Clinical examination and dermoscopy: A magnified scalp exam can identify the hallmark signs of androgenetic alopecia — miniaturized hairs of varying diameter, a widened central part with preserved frontal hairline, and peripilar (brown) casts. Dermoscopy also helps distinguish AGA from other conditions that cause diffuse thinning, such as telogen effluvium, diffuse alopecia areata, or early scarring alopecia.

Laboratory workup: Bloodwork is not always necessary for a straightforward AGA diagnosis, but it is often helpful when clinical suspicion for contributing factors exists. It is more routinely performed in women presenting with acute shedding (telogen effluvium) than in classic pattern thinning. When obtained, labs typically include a complete blood count (CBC), thyroid panel (TSH, free T4), iron panel with ferritin (ferritin levels below 40–70 ng/mL can contribute to shedding even when technically “normal”), and vitamin D. An androgen panel (total and free testosterone, DHEA-S) is reserved for women with clinical signs of androgen excess — irregular periods, acne, or hirsutism — which may suggest PCOS or another hormonal condition.
Many women presenting with hair loss have seen one or more providers who did not perform a thorough workup. A correct diagnosis is not a luxury — it is the prerequisite for effective treatment.
Premenopausal Women
For premenopausal women, the two primary anti-androgen options are spironolactone and finasteride. Spironolactone is the most commonly prescribed — it blocks the androgen receptor, preventing testosterone and DHT from acting on the follicle. Typical dosing is 100–200 mg daily. It is well-tolerated, with menstrual irregularities and breast tenderness as the most common side effects. Spironolactone is contraindicated in pregnancy, but it has a short half-life, meaning it can be stopped quickly if a patient becomes pregnant.
Finasteride can also be used in premenopausal women who want more aggressive DHT suppression and who are committed to reliable contraception. In women, finasteride is typically prescribed at 5 mg daily to more effectively reduce DHT. For maximum anti-androgen therapy, spironolactone and finasteride 5 mg can be combined. Patients must understand and formally consent to the teratogenic risk, and pregnancy must be avoided during treatment and for at least one month after discontinuing finasteride.

Postmenopausal Women
After menopause, the pregnancy concern becomes irrelevant, and oral dutasteride is almost always our preferred anti-androgen. Dutasteride blocks both Type I and Type II 5-alpha reductase, providing the most comprehensive DHT suppression available. When combined with oral minoxidil, this forms a potent two-drug regimen that addresses both sides of the equation: hormonal blockade and growth stimulation.
Oral Minoxidil
Low-dose oral minoxidil (typically 1.25–2.5 mg daily in women) has become a central component of female hair loss treatment. It prolongs the anagen phase, promotes thicker hair growth, and is more effective and far easier to maintain than twice-daily topical application — an important consideration for women with longer hair who find topical minoxidil difficult to apply and cosmetically disruptive.
Side effects are similar to those in men: hypertrichosis (excess facial or body hair) is the most common and is dose-dependent. Rarely, fluid retention can occur. Minoxidil does not have hormonal or sexual side effects.
Custom Compounding
At HMI, we use custom compounding for both oral and topical formulations to simplify treatment regimens. A single oral capsule combining minoxidil with dutasteride or spironolactone can reduce pill burden significantly. On the topical side, compounded solutions combining minoxidil at higher concentrations (5–8%) with spironolactone or finasteride can be applied directly to the scalp, reducing systemic exposure while delivering active medication to the follicular target.
Regenerative Therapy
HMI’s regenerative approach applies equally to female patients. The baseline protocol — fractional non-ablative laser (Lumenis M22 ResurFX at 1565nm) is designed to optimize the scalp environment and stimulate follicular activity.
For patients who want to be more aggressive, microneedling with Xvie exosomes or injectable PRP can be added.
At home, the Revian Red LLLT cap provides daily follicular stimulation with physician-monitored compliance. Women often respond well to regenerative interventions, particularly when combined with a solid medication foundation.

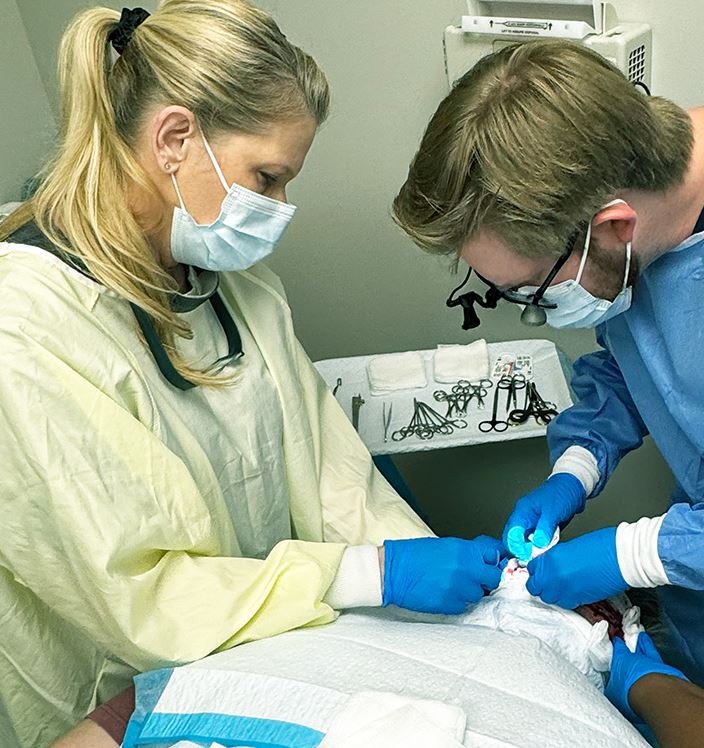
Hair transplant is less frequently discussed for women, but it is a viable and effective option in the right candidates. The key requirements are a stable donor area (the back and sides of the scalp must have adequate density and no signs of diffuse thinning that could compromise donor hair) and realistic expectations about coverage goals.
FUT (strip method) is often the preferred technique for women because it does not require shaving the head — a significant practical consideration. The resulting linear scar is hidden beneath the patient’s existing hair. For women with advanced thinning who have plateau on medical therapy, transplantation can meaningfully restore density in the areas of greatest concern — typically the central part and crown.
Having a surgeon who is also a dermatologist matters here. Accurate diagnosis ensures that a woman with diffuse alopecia areata or early scarring alopecia is not misdiagnosed as having AGA and taken to surgery with a fundamentally different condition. This distinction requires dermatologic training that most non-dermatologist hair transplant surgeons do not have.
Common Misconceptions
“It’s just stress — it will grow back.” While telogen effluvium from stress is real and self-limiting, many women presenting with diffuse thinning have underlying androgenetic alopecia that will not spontaneously improve. The distinction matters enormously, and only a proper evaluation can make it. Waiting months or years for hair to “come back on its own” when the real diagnosis is AGA means losing follicles that could have been preserved with early treatment.
“Women don’t get pattern hair loss.” They do — it is the single most common cause of progressive hair thinning in women. The pattern differs from men (widening part rather than receding hairline), which is one reason it has been historically underrecognized, but the mechanism is the same: androgen-driven follicle miniaturization in genetically susceptible individuals.
“Biotin will fix it.” Biotin supplementation is widely marketed for hair growth but has no evidence supporting its efficacy in women who are not biotin-deficient — and true biotin deficiency is rare. At best, biotin is harmless. At worst, it provides false reassurance and delays effective treatment. Notably, high-dose biotin can interfere with certain laboratory assays, including thyroid panels, potentially leading to misdiagnosis.
“I should wait until menopause to treat.” There is no clinical rationale for waiting. Hair loss treated early is more responsive than hair loss treated late. Follicles that have been miniaturized for years are far more difficult to recover than those caught in early stages. The best time to start is when you first notice thinning.
The Emotional Reality
Hair loss in women carries a psychological burden that is quantifiably greater than in men — not because the loss is more severe, but because societal norms place disproportionate emphasis on women’s hair as a marker of identity and femininity. Many women describe feeling invisible, unattractive, or anxious in social situations. Some avoid mirrors, change how they style their hair, or stop activities that expose their scalp.
Clinical validation is more powerful than sympathy. When a dermatologist examines your scalp, identifies the specific mechanism driving your loss, and presents a rational treatment plan, that itself is therapeutic. The problem has a name, a cause, and a treatment approach. You are not imagining it, and you are not powerless against it.
7 Signs You are Losing Your Hair

#1 You notice more hair on your pillow in the morning. This can be a subtle, but worrying sign that you are losing your hair.
 #2 While showering or brushing your hair, you observe an alarming amount of hair strands tangled in your brush or circling the drain, far more than the normal shedding you are used to.
#2 While showering or brushing your hair, you observe an alarming amount of hair strands tangled in your brush or circling the drain, far more than the normal shedding you are used to.
 #3 Your usual hairstyles, like ponytails or braids, feel less full, and hairband wraps around more times than it used to, signaling a decrease in hair volume.
#3 Your usual hairstyles, like ponytails or braids, feel less full, and hairband wraps around more times than it used to, signaling a decrease in hair volume.
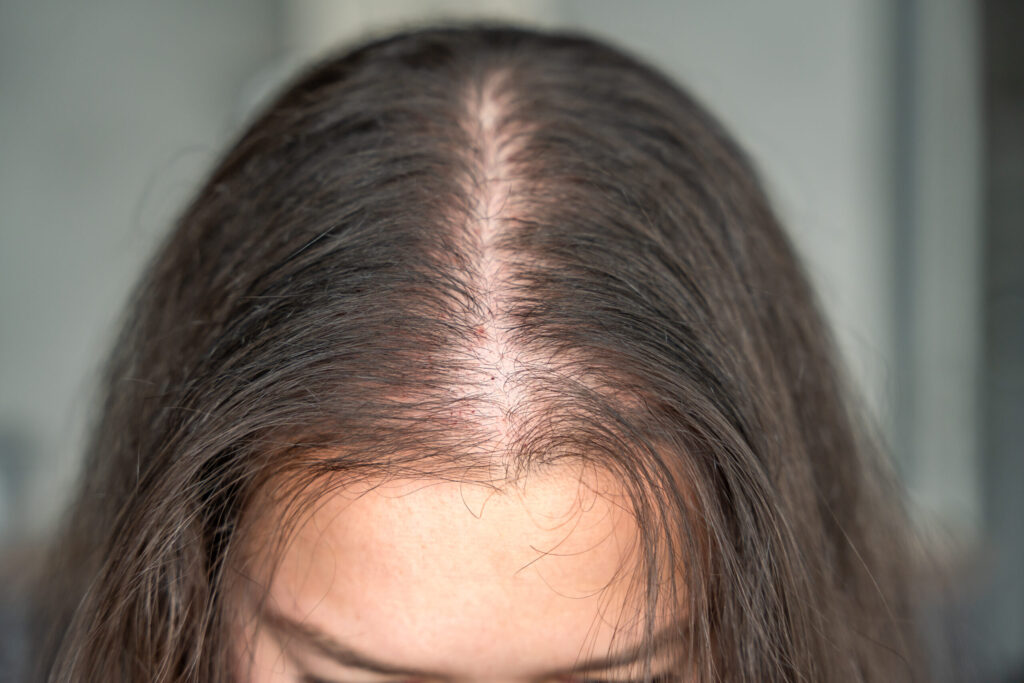
#4 You examine your scalp and notice visible thinning areas or widening parts, which were never an issue before.

#5 You start to notice that individual strands of her hair feel significantly finer and weaker than before, making your overall hair volume appear reduced and less robust.

#6 You find yourself frequently checking mirrors, trying to cover up the thinning spots with different hairstyles or products that only offer a temporary fix.

#7 You become concerned the situtation might not imporve on its own, and begin to see hair loss as not just a physical issue but one that effects you self-esteem and the way you present yourself to the world. You may feel like you've lost a part of your identity.
GET RESULTS
Hair Loss Stops Here
Women trust our evidence-based medical approach for long-lasting hair restoration.
 Assess Your Hair Loss
Assess Your Hair Loss
Receive a personalized, comprehensive physician-tailored treatment plan specifically designed for your type of hair loss.
 Start Your Treatment
Start Your Treatment
You’ll be guided through your holistic treatment plan step-by-step by our dermatologist-led care team
 Get Long Lasting Results
Get Long Lasting Results
See results within 6 months and be supported long term for a lasting solution.
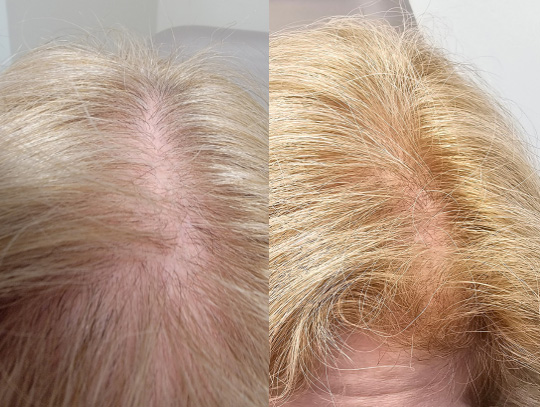
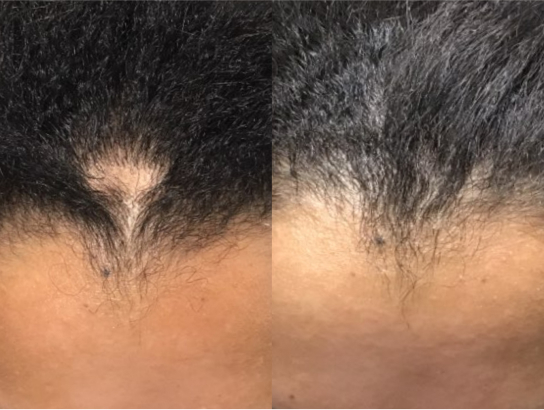
*All results at 6 months after commencement of combination medical therapy.
Without Treatment,
Your Hair Loss Will Continue.
Get a personalized treatment plan and get your hair back.
