What Is Traction Alopecia?
Traction alopecia, often referred to as hair loss on the edges, is a form of hair loss caused by chronic, repetitive pulling or tension on the hair follicle. Unlike autoimmune or hormonal hair loss, this is a mechanical problem — the follicle is physically damaged by sustained force applied to the hair shaft. It is most commonly seen along the frontal hairline, temples, and around the ears, though any area subjected to tension can be affected.
What makes traction alopecia uniquely important is that it is both preventable and — when caught early — fully reversible.
However, if the pulling continues for years without intervention, the follicles sustain permanent scarring damage and the hair loss becomes irreversible.
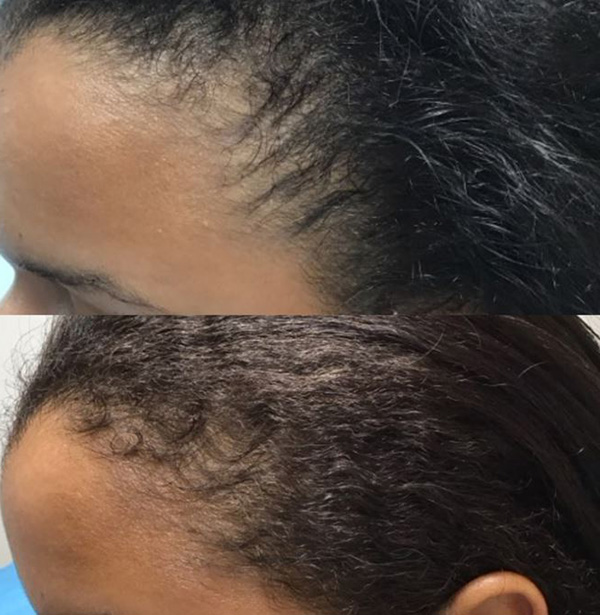
Before and after medical therapy.
Who Is Most Affected?
Traction alopecia is most common in women of African descent, driven by both the structural characteristics of tightly coiled hair and cultural hair practices that involve sustained tension. Tight braids, cornrows, dreadlocks, sew-in weaves, and extensions are well-established contributors. Chemical relaxers compound the problem by weakening the hair shaft, making it more susceptible to breakage under tension.
That said, this is not exclusively a condition of Black women. Ballet dancers who wear tight buns daily, Sikh men who wrap long hair tightly under turbans, nurses and military personnel who pull hair back for long shifts, and even children whose parents style their hair tightly can all develop traction alopecia. The common thread is chronic mechanical force on the follicle.

How Traction Damages the Follicle
When a hair is pulled repeatedly, the follicle undergoes progressive injury. In the earliest stages, the tension causes perifollicular inflammation — redness, swelling, and sometimes small pustules around the hair roots. Patients may notice tenderness, itching, or even headaches after a fresh install. These are warning signs that the styling is too tight.
Over time, if the tension continues, the inflammatory damage leads to fibrosis — scar tissue replaces the normal follicular structures. Once this occurs, the follicle can no longer produce a hair. The scalp in these areas often appears smooth and shiny, with no visible follicular openings. This is end-stage traction alopecia, and at this point, the loss is permanent without surgical intervention.
Early Versus Late Presentation
The distinction between early and late traction alopecia is the most important clinical decision point, because it determines whether the hair can come back.
Early (non-scarring) stage: The patient notices thinning or breakage along the hairline or at sites of greatest tension. Dermoscopy may reveal hair casts — small white cylindrical sheaths clinging to hair shafts — and broken hairs at various lengths. Follicular openings are still visible. At this stage, simply removing the source of tension and supporting regrowth with medication often leads to full recovery.
Late (scarring) stage: Bald patches are well-established, smooth, and devoid of follicular openings. A characteristic finding is the "fringe sign" — a thin row of retained hairs at the very front edge of the hairline, which helps distinguish traction alopecia from frontal fibrosing alopecia. Once scarring has occurred, medication cannot restore the lost hair.
Diagnosis
Traction alopecia is typically diagnosed clinically based on the pattern of hair loss and a careful styling history. A dermatologist will examine the distribution — traction alopecia follows the geography of tension, not the patterns seen in androgenetic alopecia or autoimmune conditions.
Dermoscopy can reveal supportive findings such as hair casts and broken hairs. In cases where the diagnosis overlaps with other conditions — particularly central centrifugal cicatricial alopecia (CCCA), which shares demographic and anatomic features — a scalp biopsy may be recommended to clarify the picture.
Treatment
The Most Important Intervention: Stop the Tension
No medication can overcome ongoing mechanical damage. The first and most critical step is eliminating the hairstyles and practices that are causing the problem. This does not necessarily mean abandoning all styling — it means working with a stylist to find lower-tension alternatives. Looser braids, crochet methods that reduce scalp tension, and natural styles that allow the hair to rest are all reasonable options.
Medical Therapy
For patients in the early, non-scarring phase, medical therapy can accelerate regrowth. Topical minoxidil 5% applied to the affected areas helps stimulate follicle activity. For patients who prefer a pill, low-dose oral minoxidil (1.25 mg daily) provides similar benefit with excellent tolerability. Topical or intralesional corticosteroids can reduce active inflammation, particularly during a painful or itchy flare.

Regenerative and Adjunctive Options
In select cases, regenerative therapies including microneedling with growth factor application and low-level laser therapy (LLLT) can support the recovery process, particularly in transitional areas where follicles are weakened but not yet scarred. These are adjuncts, not replacements, for the behavioral and medical interventions described above.
Surgical Restoration
For patients with established scarring who have been tension-free and inflammation-free for at least one year, hair transplantation can restore hair to affected areas. It is essential that the underlying cause has been definitively addressed before proceeding — transplanting into an area still subject to traction will result in loss of the transplanted grafts.
Talking to Your Stylist
Many patients feel uncomfortable asking their stylist to change long-standing practices. Framing the conversation around medical guidance can help: "My dermatologist recommended going looser on my edges — could we try a version of this style that pulls less at the front?" A good stylist will want to protect your hair's health and will appreciate the feedback.
Next Steps
Traction alopecia is one of the few forms of hair loss where early action can mean complete reversal — and delayed action can mean permanent loss. If you are noticing thinning along your hairline, temples, or wherever your hair is styled most tightly, a comprehensive evaluation with a board-certified dermatologist can determine whether the damage is still reversible and what treatment approach makes sense for your situation.
Without Treatment,
Your Hair Loss Will Continue.
Get a personalized treatment plan and get your hair back.
