What Is Lichen Planopilaris?
Lichen planopilaris (LPP) is a form of scarring (cicatricial) alopecia driven by lymphocyte-mediated inflammation that targets the hair follicle. Specifically, the inflammatory infiltrate attacks the infundibulum — the upper portion of the follicle where it exits the scalp — and the isthmus region where the stem cell-rich bulge is located. This location matters: when inflammation and fibrosis occur near the follicular opening and the stem cell niche, the damage is permanent. The follicle scars over, the ostium closes, and the hair cannot regrow.
LPP can present as patchy or diffuse hair loss on any area of the scalp, often with associated symptoms of itching, burning, or tenderness. It is most common in women aged 40–70, though it can occur in men and in younger patients.
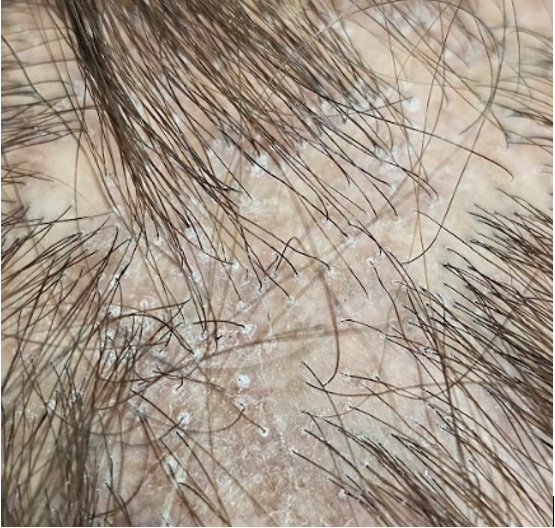
Peri-follicular scale in female mid 60s with LPP.
Frontal Fibrosing Alopecia: A Distinct Clinical Pattern
Frontal fibrosing alopecia (FFA) is a specific clinical variant of LPP in which the inflammation and scarring are concentrated at the frontal hairline. The result is a slowly progressive, symmetric recession of the hairline — the hair retreats backward, leaving a band of pale, smooth, follicle-free skin.
FFA frequently involves the eyebrows, which may thin or disappear entirely — often before the scalp involvement becomes apparent. Body hair loss, particularly on the limbs, is another characteristic feature. On close inspection, the hairline often shows “lonely hairs” — isolated single hairs that persist at the former hairline — and prominent veins on the temples become visible as the hairline retreats.
All FFA is considered a subtype of LPP. Not all LPP is FFA. The distinction is clinical: FFA has a highly characteristic distribution and clinical course that guides treatment and prognosis.
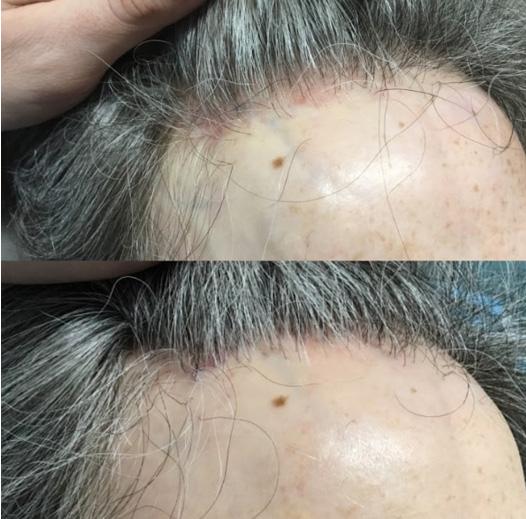
Female 50s with FFA – note the peri-follicular erythema in the before photo and the improvement in redness after treatment with oral dutasteride, a topical JAK inhibitor and topical steroid. You can also note the prominent veins in both pictures.
A Rising Incidence
FFA has increased dramatically in prevalence over the past two to three decades. While awareness and diagnostic accuracy have improved, most experts agree that the rise is not fully explained by better recognition — it appears to be a genuinely increasing condition.
This has prompted investigation into potential environmental triggers. Facial sunscreen use has received the most attention: several observational studies have reported a positive correlation between regular sunscreen use and FFA, raising the hypothesis that certain sunscreen ingredients (particularly chemical UV filters) may contribute to follicular inflammation in susceptible individuals. However, a 2020 review in the Journal of the American Academy of Dermatology concluded that there is insufficient evidence to establish a direct causal relationship. The data are suggestive but not definitive, and no one should stop using sunscreen based on the current evidence.
Other proposed triggers include contact allergens in cosmetic products, hormonal changes associated with menopause, and environmental exposures that have not yet been identified.
Symptoms and Clinical Presentation
Patients with LPP often report scalp pain, burning, or pruritus (itching) — particularly at the hairline in FFA or at the active edge of hair loss in classic LPP. These symptoms reflect active inflammation and are an important signal that the disease is progressing. Some patients describe the discomfort as a persistent tight or tingling sensation; others experience episodic flares.
Classic LPP can present with multifocal patchy hair loss anywhere on the scalp, sometimes mimicking alopecia areata on initial examination. The distinguishing clinical feature is the presence of perifollicular scale and erythema — findings not seen in alopecia areata. In some cases, LPP presents as diffuse thinning that can be confused with androgenetic alopecia, making dermoscopy and potentially biopsy essential for accurate diagnosis.
On dermoscopy, the characteristic findings include perifollicular erythema (redness encircling individual follicles), perifollicular scale (a tubular cuff of white scale around the hair shaft), and loss of follicular ostia in areas of established scarring. In FFA, the combination of hairline recession, eyebrow loss, prominent temporal veins, and lonely hairs is often sufficient for clinical diagnosis.
Diagnosis
Diagnosis is typically made by a dermatologist based on the characteristic clinical pattern and dermoscopic findings. A scalp biopsy is recommended when the presentation is atypical, when there is clinical overlap with other scarring alopecias (particularly CCCA in patients of African descent), or when the diagnosis needs to be confirmed before initiating systemic therapy.
The biopsy in LPP shows a lichenoid (band-like) lymphocytic infiltrate at the level of the isthmus and infundibulum, with destruction of the outer root sheath and progressive perifollicular fibrosis. These histologic findings distinguish LPP from other scarring alopecias that target different anatomic regions of the follicle.
Treatment
Systemic Therapy: Different First Lines for LPP and FFA
An important distinction in treatment: classic LPP and frontal fibrosing alopecia respond differently to systemic therapies, and the first-line approach at HMI reflects this.
For classic LPP, low-dose doxycycline is our first-line systemic therapy. Doxycycline has well-established anti-inflammatory properties independent of its antibiotic activity, and it is effective at calming the lymphocytic inflammation that drives LPP. It is well-tolerated, affordable, and can be used long-term as maintenance therapy once disease activity is controlled.
For frontal fibrosing alopecia, oral dutasteride is our preferred first-line agent. A recent comprehensive review of treatment outcomes demonstrated that single-agent dutasteride achieved remission in nearly two-thirds of FFA patients — a higher success rate than any other single systemic agent studied, including the historically standard hydroxychloroquine (Plaquenil). Dutasteride’s mechanism in FFA is not purely anti-androgenic; there is evidence that 5-alpha reductase inhibition may modulate the inflammatory pathways involved in follicular destruction, though the exact mechanism is still being elucidated.


Topical and Intralesional Therapy
Topical corticosteroids (high-potency solutions or foams) and intralesional corticosteroid injections remain important for controlling localized inflammation. Topical calcineurin inhibitors (tacrolimus) and topical JAK inhibitors (ruxolitinib/Opzelura) offer non-steroidal anti-inflammatory options that can be used on a long-term basis without the skin atrophy concerns associated with chronic topical steroid use.
Other Systemic Options
For patients who do not respond adequately to first-line therapy, additional systemic options include hydroxychloroquine, and in refractory cases, oral JAK inhibitors or other immunomodulators. These carry more significant side-effect profiles and require monitoring, but they can be essential for patients whose disease is not controlled with first-line agents.
Oral Minoxidil as Adjunct
Oral minoxidil is frequently added to the regimen in an effort to support and thicken hairs that are partially damaged but not yet fully scarred. It does not treat the inflammatory process itself, but it can improve the cosmetic outcome by maximizing the caliber and length of surviving hairs.
Eyebrow Management
Eyebrow loss is one of the most distressing features of FFA for many patients. Once disease activity is controlled and the condition has been stable for a sufficient period, eyebrow transplantation can be performed to restore natural-appearing brows. This is a surgical procedure in which individual follicular units — typically taken from the scalp — are transplanted into the brow area, restoring hair that grows naturally. For patients who are not surgical candidates or who prefer a non-surgical approach, cosmetic camouflage through microblading is another option. It is important that the disease is quiescent before pursuing either approach, as active inflammation in the brow area could compromise results.
Monitoring Disease Activity
Determining whether LPP/FFA is active or quiescent (“burned out”) is essential for both treatment decisions and surgical candidacy. Active disease is characterized by ongoing symptoms (pain, itching, burning), perifollicular erythema and scale on dermoscopy, and progressive hair loss documented on serial photography.
Quiescent disease shows no symptoms, no dermoscopic signs of inflammation, and stability on serial photography. Achieving and maintaining quiescence is the treatment goal. Patients are typically monitored every 3–6 months with dermoscopic photography to document stability.
Prognosis and Long-Term Outlook
LPP and FFA are chronic conditions, but they are not uniformly progressive. Many patients achieve long-term disease quiescence with appropriate therapy, and some cases appear to “burn out” over time — the inflammation resolves and the disease stabilizes, though the scarred areas do not regrow. The clinical challenge is that there is no reliable way to predict which patients will experience spontaneous remission and which will require indefinite treatment.
For patients with FFA, the hairline recession often stabilizes with treatment, though it typically does not return to its original position. Eyebrow loss may be partially reversible if treated early, but established eyebrow loss rarely recovers fully. These realities underscore the importance of early intervention: every month of untreated active disease means more irreversible follicular destruction.
Patients who have been told “there is nothing that can be done” for their scarring alopecia have often seen providers unfamiliar with the current treatment landscape. While we cannot reverse established scarring, we can stop the process, preserve the remaining hair, and in many cases significantly improve the cosmetic outcome through a combination of medical therapy, regenerative treatments, and carefully planned surgical restoration.
Hair Transplantation in LPP/FFA
Transplantation is possible in patients with documented quiescent LPP/FFA, typically after at least 12–24 months of stability on maintenance therapy. The results can be excellent, but patients must understand that LPP/FFA can reactivate, and transplanted hairs placed into a scarring environment are not guaranteed to be permanent.
Surgical planning in LPP/FFA requires a dermatologist’s assessment of disease activity. If your transplant surgeon is not a dermatologist, coordinated care with one is essential before, during, and after the surgical process.
Next Steps
If you are experiencing progressive hairline recession, eyebrow thinning, or scalp symptoms like burning, itching, or tenderness — particularly if you are a woman over 40 — a comprehensive evaluation by a dermatologist experienced in scarring alopecia is the critical first step. LPP and FFA respond best to early, aggressive treatment. The longer the disease progresses unchecked, the more follicles are permanently lost. At Hair Medicine Institute, Dr. Hawkins provides expert diagnosis, medical management, and when appropriate, surgical restoration for patients with lichen planopilaris and frontal fibrosing alopecia.
Without Treatment,
Your Hair Loss Will Continue.
Get a personalized treatment plan and get your hair back.
